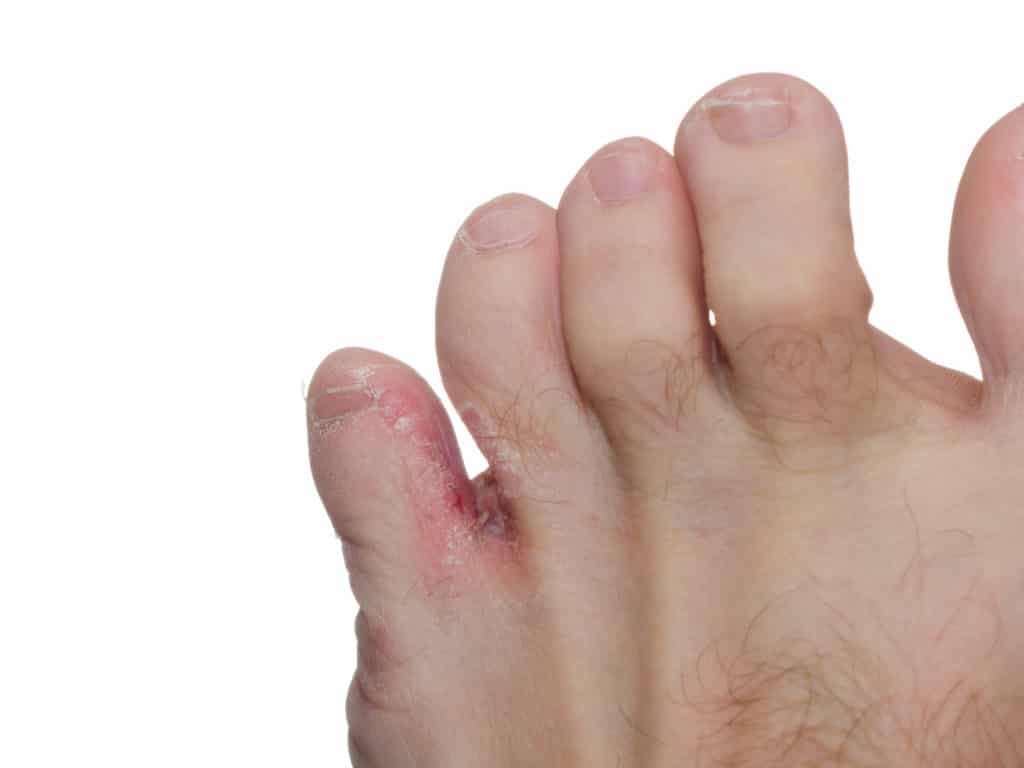
What You Need to Know About Athlete’s Foot
It may be called “athlete’s foot,” but the truth is you don’t have to be an athlete to develop this fungal infection. It’s true!
And though this annoying condition comes with a misleading name, many people are familiar with the common symptoms associated with it – the burning, itching sensation that just won’t go away. These symptoms tend to be worse immediately after removing the footwear, exposing the skin to air. However, there are other signs worth noting, like redness, scaly rashes, blisters, and even excessive dryness that can easily be mistaken for eczema.
Often, patients will start at-home treatments to get rid of what they think is a case of dry skin only to find weeks – if not months – later that what they do have is a fungal infection. That’s only one of the many reasons you should understand what athlete’s foot is and how it comes about.
So What is Athlete’s Foot?
Athlete’s foot is a fungal infection that usually starts to develop between the toes before spreading to other areas of the foot. The causal fungi are the same pathogens that cause jock itch and ringworm.
The said molds inhabit dead skin layers and prefer human hosts. Nonetheless, they can thrive in warm, damp conditions and easily transfer from one surface to another.
The skin condition is transferred through physical contact, especially from contaminated surfaces or individuals who are already infected. Although, any environment that provides warmth, low light, and moisture is a playground for fungal infestation.
Think, for instance, how hot and sweaty the inside of your shoes can get throughout the day. Or how warm and humid pool decks, locker room floors, and public showers usually are. These are all environments in which you should protect your feet to avoid picking up a nasty fungal infection. But more on that later.
Aside from being an unsightly condition, athlete’s foot is highly contagious, and virtually anyone who has feet possesses at least a certain degree of potential risk for it. (Though the condition tends to be more frequently seen in men.)
Other Risk Factors to Keep in Mind
There are other risk factors you should keep in mind, however. Some other contributors for this infection include:
- Frequently wearing tight-fitting shoes. Especially those made of materials that do not allow the feet to breathe.
- Having a weakened immune system that has an impaired ability to fight the infection. An example of this is when diabetes compromises the immune system.
- Walking barefoot in gym locker rooms, showering areas, and indoor pool decks. We know – we already touched on the subject, but it’s worth emphasizing.
- Being exposed to items that have been contaminated by an infected individual. That includes socks, shoes, and towels, as well as rugs, mats, and even bed linens!
- Previous cases of athlete’s foot
- Abnormally increased sweating also hikes the risk of athlete’s foot and makes its treatment more difficult.
As you can see, athlete’s foot doesn’t only happen to those who engage in physical activities. The risk factors involved apply to anyone who has feet and wears shoes.
There’s, however, an increased chance for those who do play sports and exercise regularly. And this makes sense when you consider that they’re spending a lot of time in locker rooms and that their feet become sweaty as they try to stay cool during intense activity.
Where can you get athlete’s foot?
Being contagious, you can contract athlete’s foot when you contact contaminated surfaces or infected persons.
As mentioned, the causal fungi thrive in damp and warm atmospheres. That makes locker rooms, saunas, and swimming rooms high-risk areas.
Fungi can rub off bare feet and fingers or inhabit dead skin – continually falling off the body. Infested skin particles may spread to shoes, socks, clothes, beddings, pets, and other people’s belongings. Think of bathtubs, sinks, showers, counters, rugs, floors, towels, and carpets.
Improperly cleaned pedicure instruments can also spread the infection.
What areas of the body can be affected by Athlete’s foot?
The fungus responsible for causing athlete’s foot can infect any part of the foot. Often, the fungus grows between the toes and spread to other areas.
Generally, athlete’s foot can affect:
- The bottom of the foot
- Toenails
- Fingers
- Fingernails
- Hands, chests, arms, and other body parts
Symptoms of Athlete’s Foot
The athlete’s foot often manifests as fissures or patches between the toes.
As the condition progresses, it may cause the skin to become itchy, turn red, and appear moist. Blisters may spread from the toes to the soles of the feet, swelling and breaking to expose painful raw fissures.
When the infection spreads to the toes, it may cause them to appear thick and whitey or cloudy yellow.
In advanced cases, the resulting rash will extend across the sole – causing your feet to develop a foul odor and ooze pus.
In a nutshell, the common symptoms of athlete’s foot include:
- Scaly, cracked, or peeling skin
- Itchiness, particularly right after taking off socks and shoes
- Blisters
- Burning or stinging
- Inflamed skin (which may appear reddish, grayish, or purplish depending on your skin color)
- Dry, scaly skin on the soles that extends up the side
If you portray these symptoms, you likely have the infection. But we may need to perform tests to be sure.
Treatment Options for Athlete’s Foot
In case of a mild condition, home treatment should be your first choice. Well, unless you have diabetes or a weakened immune system. In which case, you should contact Dr. Timson first.
Home treatment typically involves washing your feet thoroughly at least once a day. (Followed by topical application of the available over-the-counter antifungal sprays or creams, such as Loprox, Penlac, Ecoza, or Lotrisone.)
Follow the instructions stipulated on the package and complete the treatment course fully for best results. Don’t stop when the symptoms disappear ahead of schedule. Continue the treatment for 2-6 weeks after the symptoms clear up, or until all the affected skin layers are replaced.
Be sure to treat all the affected areas – it could be hands, torso, or toenails. The idea is to prevent the infection from spreading to treated areas.
Treating just the infected area is not enough. Once your shoes or socks are infested with the causal fungus, they can re-infect the treated area if worn again. To prevent reinfection:
- Clean the socks by adding bleach in the water or using water warmed to 140°F or above.
- Treat your shoes with antifungal spray or powder, or
- Dispose of infected socks and shoes
If the condition does not respond to self-care and nonprescription products: see a medical professional. The same goes if the infection is severe or has excessive redness or swelling, or if it causes fever.
Diagnosis
When you come to Dr. Timson, we’ll first confirm the diagnosis. That may involve taking a sample of your skin for lab analysis.
If the infection is confirmed, we may prescribe a stronger antifungal medication than over-the-counter creams. We may prescribe antifungal pills like Lamisil, Tolsura, and Sporanox.
Other medications, like oral antibiotics or topical steroids, or oral antibiotics, may be provided to: manage symptoms and control secondary bacterial infections.
When using antifungal products, follow the instructions carefully for optimal efficiency. Symptoms will start to clear up before the condition is treated completely. But this doesn’t mean the infection has been completely eradicated – make sure to follow the listed directions concerning the length of treatment, too.
Additionally, we will want to talk with you about your lifestyle, your activities, or even your shoes to identify any potential risk factors causing the infection and give you the guidance you need to prevent it in the future.
Preventing Athlete’s Foot
But even better than treating an irritating case of athlete’s foot is to prevent it from happening in the first place! And you can if you:
- Wear clean and waterproof shower shoes or sandals whenever walking through high-risk areas.
- Never share socks, shoes, or used towels and beddings with anyone else (including family members).
- Use antifungal spray or powder on your feet and in your shoes. Proven options include Lotrimin AF and Lamisil AT; however, you should experiment to find formulations and products that work for you.
- Change socks often (especially when the pair you are wearing becomes damp). You can also opt for moisture-wicking socks like those made from cotton to keep your feet dry longer.
- Wear shoes made from breathable materials, like leather, nylon mesh, etc.
- Alternate between two pairs of shoes, allowing a 24-hour window for the shoes to dry completely between uses.
- Thoroughly wash your feet daily, paying attention to those areas between the toes.
Say Goodbye to Itchy, Burning Feet
For more information about athlete’s foot, treatment for fungal infections in your lower limbs, or to request an appointment for any of the comprehensive podiatric treatments, please don’t hesitate to give us a call!
If you prefer to reach us online: take advantage of our request form, too!
McPherson Office
316 W. 4th Street
McPherson, KS 67460
P: (620) 241-3313
F: (620) 241-6967
© Community Foot Clinic of McPherson. All Rights Reserved.
Privacy Policy | Terms & Conditions
Web Design by CP Solutions
Marketed by VMD Services